G. M. Naidu (University of Wisconsin-Whitewater), Atul Parvatiyar & Jagdish N. Sheth (Emory University, Atlanta), Lori Westgate (HCIA Inc., Baltimore) | Relationship marketing has been gaining momentum as business entities realize that short-term sales/transaction orientation has several pitfalls for building customer loyalty and continued patronage. Relationship marketing has the potential to improve marketing productivity (Sheth and Parvatiyar, 1995a). Development and implementation of customer retention programs, partnering with customers, suppliers, and competitors, and other relationship marketing practices have become a way of life in the 1990s. What is the nature of relationship marketing practices adopted by hospitals in the United States? How do these practices correlate with the performance of such hospitals? These and related issues are the focus of this empirical investigation
Introduction
Faced with mounting pressures to contain costs and mandates to adopt continuous quality improvement processes, the health care industry is actively engaged in relationship marketing and relational partnering activities. Many of them have created integrated delivery networks and in alliances and partnering relationships with other hospitals, physicians, HMOs, PPOs, insurers, patients as well as their suppliers. For example, in 1993 alone, hospitals formed more than 300 collaborative ventures. According to HCIA – DeLoitte and Touche’s survey, in 1995, about 81 percent of 1,191 hospital respondents said that they either participate in or have agreements with HMOs, which compared to 1992 response was 11 percent higher, and compared to 1986 survey indicated a 33 percent increase in such agreements (HCIA and DeLoitte and Touche, 1995). A survey of the 50 HMO plans by the Group Health Association of America (GHAA) survey revealed that 75 percent of them had formed or plan to form new affiliations with hospitals, physicians, PHOs, or other providers in 1995 (HCIA and DeLoitte and Touche, 1995).
The growing trend of partnering with customers, suppliers and other service providers in the health care sector, is largely driven by the competitive intensity currently facing hospitals as well as by the need to reform the health care delivery system or face the risks of closure. With improved medical technologies, in-patient days are declining and out-patient admissions are increasing, resulting in an overcapacity of beds and lower occupancy rates for hospitals. Throughout the 1980s, the average number of beds per hospital has declined along with lower occupancy rates. During the past decade (1985 – 95), more than 100 hospitals per year have closed their doors. The mortality rate of rural hospitals is almost twice that of urban hospitals (AHA, 1995).
Thus, with increased competition and improved technologies, survival has become the name of the game in this industry. To survive, hospitals have to be more productive in meeting the health care needs of the people. With growing customer demand for quality health care service, many hospitals are seeking opportunities to engage in partnering relationships with other hospitals, physician groups, HMOs and similar health care providers so that they can share their resources and capabilities, thereby increasing efficiency in the system (Trombetta, 1989). Hospitals also see the opportunity to enhance their effectiveness as partnering with other health care providers provides the capability to fully meet the needs of individual customers. Also, understanding individual customersí needs become easier when long-term relationships exists and are leveraged for longitudinal information about the customersí general and particular health conditions (Gould, 1988).
Several other factors are also facilitating hospitals to engage in relational partnering and relationship marketing activities. For example, the deployment of ëfront-line information systemsí (FIS) and the application of modern technology are making it easier for hospitals to conduct ëreal timeí diagnostics, shorter lab tests, and provide remote access to patient information. They can utilize the facilities and expertise of other health care providers; cross-sell each otherís products/services; co-design and co-market new programs; instantaneously retrieve, update and share patient/customer information; engage in after marketing to provide post-treatment satisfaction; and offer full-line health care delivery programs to customers and corporate clients through channel integration.
Thus, relationship marketing, which can be defined as the ìprocess of developing cooperative and collaborative relationship with customers and other market actors,î (Sheth and Parvatiyar, 1995b), is being increasingly practiced by hospitals. As this practice grows it is important to assess whether such activities and programs result in improved performance. No empirical study has been conducted, as yet, to determine whether it pays for hospitals to engage in relationship marketing. It is the objective of this exploratory study to assess the performance of US hospitals that engage in relationship marketing. This empirical study, based on a national sample, examines the nature of relationship marketing hospitals are currently practicing and relates these practices with the hospital’s overall performance.
Literature Review
Today, relationship marketing is at the forefront of academic research and marketing practice (Berry, 1995; Parvatiyar and Sheth, 1996). However, much of the current research has focused on defining constructs and presenting conceptual models of relationship marketing or identifying key moderators of successful relationships, such as trust and commitment (Morgan and Hunt, 1994). Several studies have been applied in the context of business-to-business marketing (Dwyer, Schurr, and Oh, 1987; Johanson, Hallèn, and Seyed-Mohamed, 1991; Wilson, 1995), or in channel relationships (Boyle, et. al., 1992; Ganesan, 1994; Weitz and Jap, 1995), or specific service industries (Crosby and Stephens, 1987; Crosby, Evans, and Cowles, 1990), etc. However, no research, with the possible exception of Kalwani and Narayandas (1995) in which the authors found a positive correlation between long-term relationships and profitability of suppliers, has yet empirically demonstrated the association or correlation between a company’s adoption of relationship marketing programs and its performance.
The relevance of relationship marketing in health care has been widely recognized (Cassidy, et. al., 1993; Dunn & Thomas, 1994; Naidu et. al., 1994; MacStravic & Denning, 1986; Paul, 1988). Wagner, et. al. (1994) discussed the relevance of relationship marketing programs, integrated marketing communication strategy, and data base marketing for developing a favorable image leading to improved hospital performance. Based on Demmingís principles of total quality, Doyle and Bondreau (1989) advocated hospital-supplier partnerships as a means to improve productivity, to control costs, and to improve quality of care. They suggest that long-term relations with suppliers based on trust, service, and effective coordination could lead to efficiencies and improved performance. Dunn and Thomas (1994) draws clear distinction between transaction selling and offering partnership solutions to customer problems and advocated partnering with customers with a hierarchy of corporate buying-selling model.
Several marketing practices that attempts to establish, develop, or maintain cooperation and collaboration with customers, and other marketing providers are included under the general rubric of relationship marketing. These include aftermarketing activities (Vavra, 1992), one-to-one marketing (Pepper and Rogers, 1994), membership programs (including frequent buyer incentives), cross-distribution arrangements, cross-selling, co-production, co-branding, channel partnerships, logistics sharing, special supply arrangements (including special sourcing, and JIT arrangements), business alliances, database marketing, etc. (cf. Sheth and Parvatiyar, 1995b).
In the health care context, hospitals could engage in cooperative and collaborative arrangements with several groups of customers including, patients, payers and HMOs or PPOs. They could also partner with their suppliers, other hospitals and/or specialized health care service providers to enhance their offerings to customers. These arrangements could be broadly classified into three types of relationship marketing practices: (1) programs that are aimed at customer retention, (2) programs that involve special supply and delivery arrangements with other health care providers and key suppliers, and (3) relational partnering programs to leverage the resources of others. Customer retention programs may include such activities as, after-marketing and post-treatment satisfaction services, frequent user benefits, patient focused care programs, database maintenance, support for on-going relationship with customers, and programs to involve customers into the design, development and sales activities of the hospital. Special supply and delivery arrangements could involve such sourcing arrangements as just-in-time supply, preferred vendor programs, membership in health care networks, integrated delivery systems, cross-selling and mutual referral of services, and sharing of patient information with other health care providers. When hospitals are interested in leveraging the resources of their partners they may engage in, joint marketing/training programs, joint product/ process development, cross distribution arrangements, logistics/ facilities sharing, co-providing services, joint ventures and alliances.
Sheth and Parvatiyar (1992) suggest that alliances and partnering arrangements are formed either for strategic or operational purposes. Strategic purpose alliances strive to improve the effectiveness of the organization by providing entry into new markets, help develop successful new products, improve the hospitalís market position, and help in achieving rapid acceptance of new marketing programs by its customers. These in turn should increase customer loyalty and further improve the market position of a hospital. Operative purpose alliances are aimed at increasing marketing and organizational efficiency of the hospital by reducing operating and developmental costs, reduce cycle time for introducing new and innovative products, achieve quality benchmarks, increase productivity and improve the hospital’s operating processes, etc. As indicated by Turner and Pol (1995), many US hospitals are taking patient satisfaction, quality of care, integrated delivery and health care costs seriously and are adopting measures towards accomplishing them to become more effective and efficient.
Research Hypotheses
Our objectives in this study are: (i) to determine the antecedents of the degree to which a hospital engages in relationship marketing; and, (ii) to determine the impact of relationship marketing activities on a hospitalís performance. Figure 1 represents the theoretical model under investigation. Its central premise is that the degree to which a hospital engages in relationship marketing activities will be dependent on the competitive intensity faced by the hospital, the hospitalís marketing orientation and the presence or abscence of a marketing department in the hospital. Consequently, the degree of relationship marketing activities adopted would impact the hospitalís performance in terms of its occupancy rate, admissions per bed, uncollectible ratio, and the gross patient revenue per patient day.
Antecedents to the Degree of Relationship Marketing Activities
Although there might still remain significant barriers that impede end users (patients) from switching, the hospital market is shifting from a market dominated by semi-monopolies to one characterized by intense competition. There are now moments when the switching barriers drop and patients can and do switch hospitals if they are not fully satisfied (Jones and Sasser, 1995). Under these circumstances, many hospitals are engaging in relationship marketing to strengthen the satisfaction-loyalty relationship with patients, and further influence physicians, HMOs or insurers to deliver patients to them. According to Sheth (1994), the greater the competitive intensity faced by a company, the greater is its desire to cooperate and collaborate with other industry partners. As competitive forces lead to loss of customers, there is a growing need to retain these customers. Reicheld and Sasser (1990) have demonstrated across a variety of service industries that when a company successfully lowers its customer-defection rate, its profits climb steeply. This becomes a strong motivation for hospitals to engage in relationship marketing activities.
Hypothesis 1: The greater intensity of competition faced by a hospital, the greater its relationship intensity.
Other studies, though not directly related to relationship marketing have emphasized the need for a market orientation and a more targeted marketing approach for hospitals. MacStravic (1984) advocated market segmentation based on customers’ needs that strive to anticipate and exceed customers’ expectations. O’Connor, et. al. (1994) identified through an empirical study that there is a gap between what the physicians think as service quality and customer expectations of service quality. They suggest that niche marketing and relationship marketing programs must be linked by a comprehensive data base. Thus, we expect that hospitals that have a greater marketing orientation are likely to have a higher degree of relationship marketing activities.
Hypothesis 2: The greater the marketing orientation of a hospital, the greater its relationship intensity.
Relationship marketing practices are often dependent on the marketing executive who is knowledgeable about current trends and practices not only in health care but also in the entire business world. Often, such talent may be hired by larger hospitals who have an organizational slot for functional responsibilities. These functional responsibilities are often vested in the marketing departments and talented marketing executives are housed therein to formally organize the marketing activities of the hospital. Thus, we expect that in hospitals with formal marketing departments there will have a greater degree of relationship marketing activities.
Hypothesis 3: To the extent there is a formal marketing department in a hospital there will be a greater relationship intensity in that hospital.
Impact of Relationship Marketing Activities on Hospital Performance
It has been argued that relationship marketing improves a firmís productivity (Sheth and Parvatiyar, 1995b; Sheth and Sisodia, 1995). That is to say, relationship marketing must result in improving the general and specific performance indicators of a hospital. If relationship marketing activities do not result in improving the bottom-line, its likely continuation in the future will be seriously impeded. As far as the performance of a hospital is concerned, several financial and non-financial indicators have been used in various studies in the past. McDermott, et. al. (1993) used operating margins as an indicator of hospital’s profitability, and hence performance. Naidu, Narayana and Pillari (1991) and Naidu, Kleimenhagen and Pillari (1994)
have used a variety of financial and non-financial measures, such as occupancy rates, gross patient-revenue per bed, return on assets, average admissions per bed, etc., to evaluate the performance of hospitals. The use of financial and non-financial measures to evaluate business performance is consistent with the recommendations made by Eccles (1991).
In a declining market, one of the major problems faced by hospitals is decreased utilization of bed size capacity. On a typical day, more than one-third of the hospital beds are empty. Improved procedures, greater emphasis on out-patient services, and pressure to contain costs have contributed to lower patient-days per hospital admission. On one hand this may be good for patients and payers, but hospitals who have to bear significant overhead costs due to under-utilization of capacity, may find their bottom line severely affected due to low occupancy rates. However, if relationship marketing is aimed at retaining customers and facilitating future marketing activities, hospitals that engage in them are likely to see a relative superiority in maintaining its occupancy rates over other hospitals. Such hospitals will also draw more patients given the satisfaction of those who have previously been served by them and the subsequent favorable word-of-mouth publicity.
Closely related to occupancy rate is another performance indicator – admissions per bed. Relationship programs with customers, such as HMOs/PPOs/physicians/payers directly enhance the opportunities for repeat purchases and increased loyalty. Not only will these HMOs, PPOs, physicians and others recommend their patients, other patients and customers will also be attracted to the hospital due to the favorable image generated by relationship marketing programs.
Given the time lag and general policy of hospitals that patients do not necessarily pay at the time they receive hospital services, and also the fact that most users of hospital services are not direct payers themselves, uncollectible ratios could be significant and become a cause for major financial problems for hospitals. It is expected that hospitals who engage in partnering relationships with its customers, HMOs/PPOs/physicians, payers, and suppliers are likely to experience lower uncollectible ratios than those that do not practice relationship marketing.
Customers are likely to be more responsive towards meeting their responsibilities of payment for services when they have a long-term relationship with a particular hospital. They are likely to be more motivated towards maintaining the financial health of their favorite health care facility so that they can continue to receive superior service.
Selectively targeting at the more profitable customers is one of the ways to practice relationship marketing. By tailoring customer service to profitable customers and by instituting patient focused programs, hospitals should be able to increase their gross patient revenue per patient day. Gross revenues should also increase because of improved customer satisfaction and customer loyalty in relationship marketing.
Hypothesis 4: The greater the relationship intensity of a hospital, the higher would be its performance, as measured by its occupancy rate, admissions per bed, gross patient revenue per patient day, and lower uncollectible ratio.
Research Methodology
A survey instrument consistent with the objectives of the study was developed and pretested. The eight-page survey was divided into three parts: Part A dealt with relationship marketing practices with customers and suppliers; Part B dealt with marketing organization and orientation; and Part C primarily dealt with background information of the hospital and the respondent.
A stratified random sample of 1,231 hospitals were drawn from the HCIA data base covering a cross-section of all states and bed size. A supplemental sample of 448 hospitals were drawn from the 1994 AHA Guide to experiment on a limited basis the responsiveness to incentives. A personalized letter addressed to the hospital administrator was sent in August of 1994, along with a reply envelope. A follow-up mailing was sent in September. Approximately 14 surveys were returned to the sender undelivered; 34 hospitals did not want to participate; and 26 were partially completed and judged to be unusable. This resulted in 205 usable responses (response rate of 12.8 percent) which served as the database for the study.
Secondary data related to performance indicators, such as admissions per bed, gross revenues, and other select financial ratios, were requested from HCIA for these 205 hospitals. Eighteen hospitals could not be located on the HCIA data base as these were smaller hospitals that were not recognized for Medicare/Medicaid programs and, as such, were not required to disclose their financial data. This resulted in a full set of 187 hospitals on which we have extensive primary data as well as secondary data pertaining to performance indicators.
Operational Definitions
Relationship Intensity:
The survey instrument listed 11 popular relationship marketing activities with an option to list other activities not listed therein. Respondents were asked to check as many applicable activities for which their hospital have specific programs. Based on the number of activities checked, and by dividing the sample into three fractiles using the number of activities as scores, the following operational definition of relationship intensity is used:
| Number of programs checked | < 4: | Low intensity/level |
| 5-7: | Moderate intensity/level | |
| > 8: | High intensity/level |
Marketing Orientation:
The survey listed 18 statements related to management philosophy and marketing orientation. Respondents were requested to rate each item on a scale, zero to ten (0=hospital does not possess the characteristic,…,10=hospital posses the characteristic to the maximum possible degree). The total score obtained by summing the 18 items is defined as follows:
| Total score | < 79: | Low marketing orientation |
| 80-124: | Moderate marketing orientation | |
| > 125: | High marketing orientation |
The cutoff points are defined by arranging the range of scores into three fractiles, so as to contain at least 25 percent of the observations in any category and to facilitate minimum requirements for the chi-square analysis.
Intensity of Competition:
Respondents were asked to indicate overall competitive intensity in their service area: Nonexistent, moderate, intensive, or very intensive. This is a subjective measure based on the perception of the respondent.
Performance Indicators:
The following definitions are directly obtained from HCIA data base used for this study: Occupancy rate = [Inpatient days/ # of beds x 365] x 100
Admissions per bed = (# of Admissions, Acute Care)/(# of Beds in Service) Net income margin = [(Net Income)/(Total Operating Expense)] x 100
Gross patient revenue per patient day = (Gross Patient Revenue)/(Adjusted Patient Days) Total profit margin (%) = [(Net Income)/(Net Patient Revenue + Other Revenue)] x 100 Uncollectible ratio: = [(Gross Patient Revenue – Net Patient Revenue)/(Gross Patient Revenue)] x 100
Profile of Respondents
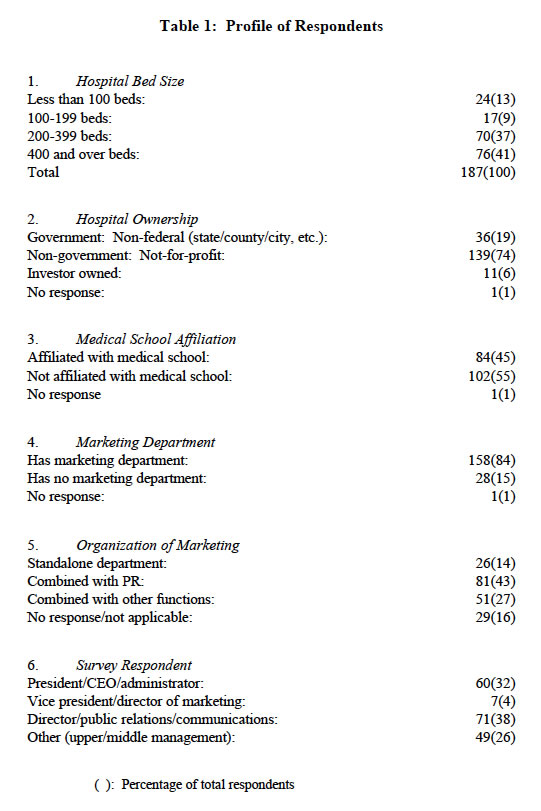
About 22 percent of the respondents represented hospitals with less than 200 beds; 37 percent were hospitals with 200 to 399 beds; and 41 percent represented general hospitals with 400 or more beds (Table 1). Nearly three-quarters (74 percent) represented “not-for-profit” hospitals and 19 percent were government (non-federal) hospitals and six percent were “investor-owned” hospitals. About 45 percent of them were affiliated with a medical school. Some 84 percent of them had a marketing department and one-in-six was a stand-alone department with the rest either combined with public relations or strategic planning or other functional areas. About one-third of the respondents were hospital Administrators/CEO/president and the balance were top management personnel (vice president, director, manager).
Analysis and Results
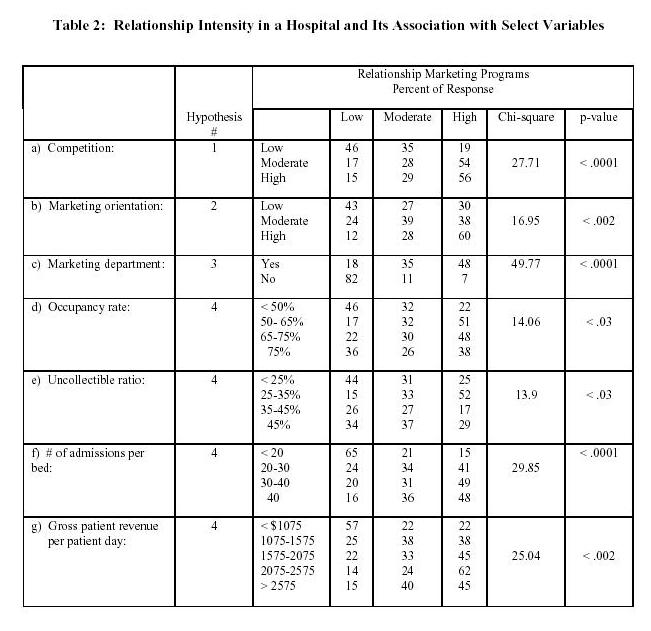
Table 2 presents results of the chi-square test of association for the study variables. The hypotheses suggest that there should be a positive association between the intensity of competition, the level of marketing orientation, and the existence of a marketing department with the level of relationship intensity in a hospital; and the level of relationship intensity should be positively associated with the hospitalís performance level on each of the following performance indicators: occupancy rate, admissions per bed, gross patient revenue per patient day, and lower uncollectible ratios. The hypotheses were investigated with the chi-square test of association that included a significance test by calculating the p-value to determine the probability of the variables being positively associated by chance. A p-value below 0.05 would imply that there is a significant relationship between the variables as predicted in the hypothesis.
The results indicate that intensity of competition and relationship intensity are not independent and that relationship intensity increases significantly when competition is high and/or moderate. This relationship between level of competition and level of relationship marketing programs is significant at a p-value of less than 0.0001. Although there is no causality established by the association tests conducted here, subsequent interviews with some hospital managers revealed that as the level of competition intensifies, hospitals tend to initiate partnership/cooperative programs with customers, HMOs/PPOs/physicians, payers, and suppliers.
Table 2 also shows the percentage distribution of responses by marketing orientation and level of relationship intensity of the hospital. The chi-square test here indicates that these two variables are associated and their association is significant at a p-value of less than .002. Hospitals that are marketing and customer-oriented initiate and maintain several relationship marketing programs that are consistent with this management philosophy. Further, it is clearly inferred from Table 2 that 83 percent of the hospitals with a marketing department have moderate or high relationship marketing intensity as compared to only 18 percent for hospitals with no marketing department. The relationship is highly significant with a p-value of less than 0.0001.
The results also suggest that hospitals engaged more in relationship marketing activities tend to have better occupancy rates. Below 50% occupancy is most prevalent among hospitals that have low intensity of relationship marketing, whereas higher levels of occupancy is more prevalent among hospitals that have high relationship marketing intensity. Low levels of relationship marketing activities had an occupancy rate of 63.5 percent as compared to hospitals with a higher level of relationship marketing activities that had an occupancy rate of 65.2 percent. The relationship between higher occupancy rates and higher level of relationship intensity is significant at p-value of less than .03.
Once again, Table 2 indicates that there is a significant relationship (p-value less than 0.0001) between number of admissions per bed and the level of relationship marketing activities in a hospital. The median admissions per bed in a hospital with low levels of relationship marketing is 25.7 percent as compared to 35.5 percent for hospitals with higher levels of relationship marketing programs. From the table it is clear that over 80% of hospitals that registered more than 30 admissions per bed have moderate to high relationship marketing intensity.
Relationship intensity and lower uncollectible ratios are related with a p-value of .03. The median percent of uncollectible ratio for hospitals with a low intensity of relationship marketing activities is 36.5 percent as compared to 34.4 percent for hospitals with a high level of relationship marketing intensity. However, it is worth noting that the lowest level of uncollectible ratios (less than 25%) is most common among hospitals that have low level of relationship marketing activities. This maybe because hospitals that are not that customer relationship-oriented could be driven by short-term financial results and are aggressive in collecting service charges as soon as possible without caring that much about their long-term relationship with customers and/or patients.
As evidenced in Table 2, relationship intensity and gross revenue per patient day is significantly related with a p-value of less than .002. The mean revenue per patient day is $1,300 for hospitals with a low intensity of relationship marketing activities as compared to $1,862 for those with a higher intensity of relationship marketing activities. About 57% of hospitals who gross less than $1075 per patient day have low relationship marketing intensity, whereas 85% of hospitals that gross over $2075 per patient day have either moderate or high relationship intensity. Based on the above results, we can conclude that the level of relationship marketing activities of a hospital and their performance on financial and non-financial indicators are positively associated.
Relative Impact of Partnering Specific Partnering Programs
In addition to the main effects study of the degree of relationship marketing activities, its antecedents and consequences on bottom-line performance variables, the study also investigated the impact of individual partnering programs initiated by a hospital on its overall performance. Although no formal hypotheses were developed, it is instructive to examine the association between specific partnering programs and individual performance indicators. Respondents were asked to check the specific partnering programs with customers, suppliers, and/or other health care providers from a list of eighteen programs mentioned in the survey instrument (with an option to list other programs not mentioned therein). Using each of these programs as study variables, and several indicators of hospital performance, such as occupancy
rate, admissions per bed, net income margin, gross patient revenue per patient day, total profit margin and uncollectible ratio, a chi-square test of association was performed.
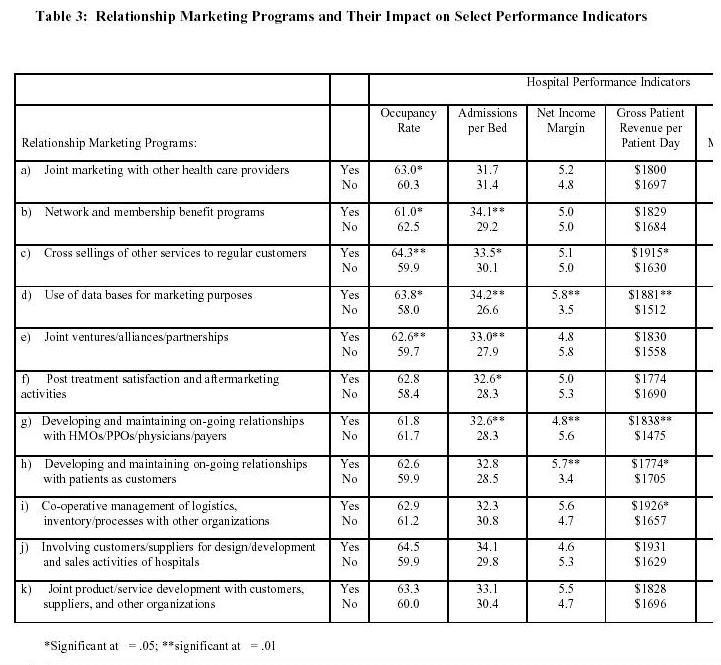
The association of specific relationship marketing programs with several performance indicators is shown in Table 3. As the results indicate, many relationship marketing programs are associated with several performance indicators. For example, ongoing relationship with patients as customers have an impact on gross patient revenue per patient day, net income margin and total profit margin. Similarly, relationships with HMOs/PPOs/physicians and payers significantly impact the hospitalís admissions per bed as well as its gross patient revenue per patient day. However, these relationships are also significantly associated with lower net income margin of hospitals, suggesting that managed care relationships may often involve ìdeep discountsî, ìcarve outsî and ìcapitation feesî to physicians, PPOs and HMOs.
Use of databases for marketing purposes have wide ranging impact on several performance variables including, occupancy rates, admissions per bed, net income margin, gross patient revenue per patient day, and total profit margin. Higher occupancy rates, higher number of admissions per bed, and improvement in gross revenue per patient day are found in hospitals that engage in cross-selling other services to regular customers. Occupancy rates and admissions per bed are higher in hospitals that engage in programs to provide network and membership benefits. Similarly, lower uncollectible ratio and higher number of admissions per bed are found in hospitals that engage in after-marketing and post-treatment satisfaction services. Hospitals that engage in joint marketing programs with other health care providers have higher occupancy rates, whereas cooperative management of logistics impacts the gross patient revenue per patient day. Finally, hospitals that engage in joint ventures and alliances with other health care providers also achieve a higher utilization of their facilities through high occupancy rates and higher admissions per bed, at the same time maintaining lower uncollectible ratio.
Two programs that have no significant association with any of the six performance indicators tested are: (i) involving customers/suppliers for design/development and sales
activities of hospitals; and (ii) joint product/service development with customers, suppliers and other organizations. This maybe due to the fact that unlike manufacturing and consumer service organizations, customers usually rely on the expertise of the health care professionals for the design and delivery of care services. There is less enthusiasm among customers to become involved in the process of design or development of new products and services at hospitals.
Relative Impact of Partnering with Customers, Suppliers and other Health Care Providers
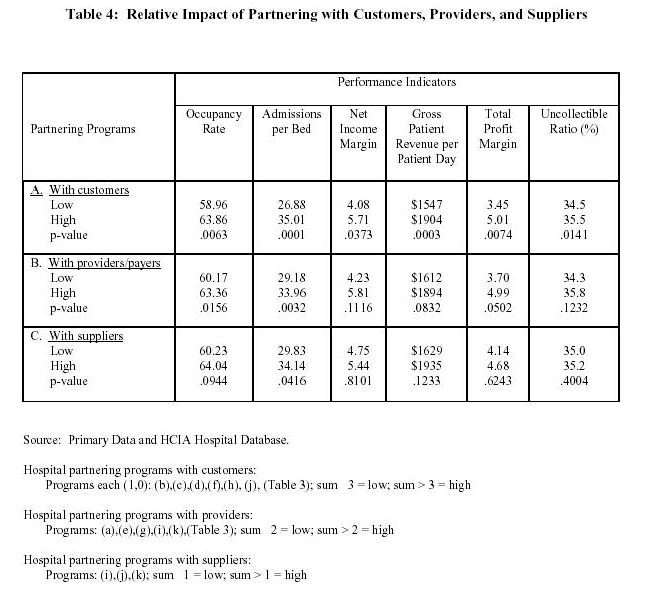
Since relational partnering programs are developed with customers, suppliers and other health care providers or payers, etc., knowing their relative impact on a hospitalís performance could be useful in planning future programs. It could also help in developing realistic expectations as to what results should be expected from different types of partnering programs. To consider relative impact on performance of partnering with customers, providers/payers, and suppliers, several relational partnering programs were summed over the binary scale (1,0) and low and high levels of partnering programs were operationally defined. These were then associated with six performance indicators: occupancy rate, admissions per bed, net income margin, gross patient revenue per patient day, total profit margin, and the uncollectible ratio.
As shown in Table 4, those who are engaged in a higher level of partnering with customers have better overall performance. On all six performance indicators, hospitals with a higher number of partnering programs with customers performed significantly better than those who had a lower number of partnering programs with customers. The most significant difference in performance between those who have high levels of customer partnering versus those that have less are in the areas of occupancy rates achieved, admissions per bed, gross revenue per patient day earned and the total profit margin. The least difference appear in the areas of net income margin and in the uncollectible ratio. This could be because of the high costs of running multiple partnering programs with customers and also because focus on building long-term relationship with customers may be associated with compromises on short-term profitability.
As shown in Table 4 (Row B), partnering programs with providers and payers contribute to higher utilization of facilities (occupancy rate and number of admissions per bed) but has marginal impact on financial performance indicators. A couple of financial performance indicators such as profit margin and gross patient revenue per patient day are marginally significant with p-value of 0.05 and 0.08. This may imply that in the short term partnering with other providers may have an anemic impact. However, hospitals can benefit in the long run through better utilization of facilities as more patients are brought through partnering arrangements with HMOs and PPOs.
The incidence of hospital partnering with suppliers is less prevalent and so is its association with overall performance indicators. Only hospital facilities utilization (occupancy rate and admissions per bed) and supplier partnering are associated and that too at marginally significant levels. This association itself may be due to concurrent partnering programs with customers and payers. Several explanations can be provided for this lack of strong association between supplier partnering and a hospitalís overall performance. For example, relative to the hospital budget, the supplier budget in some cases may be too small to have a significant impact on financial performance indicators of the hospital. Or, it is possible that the relative unsophistication in supplier partnering may not have yielded significant results as yet. However, partnering with suppliers do have the potential to provide such benefits as reduction in procurement costs, lower developmental costs, etc., that we have not measured here. Thus, even though the chi-square test results indicate that supplier partnering and overall hospital performance are independent, a different set of measures could prove otherwise.
Limitations of the Study
The above analysis is exploratory in nature and cause and effect of these programs on the performance of a hospital cannot be directly established. They only demonstrate a positive association between relationship marketing activities and programs and performance indicators. Using this study method of a cross-sectional survey at only one point in time, we can only hope to detect associations between variables.
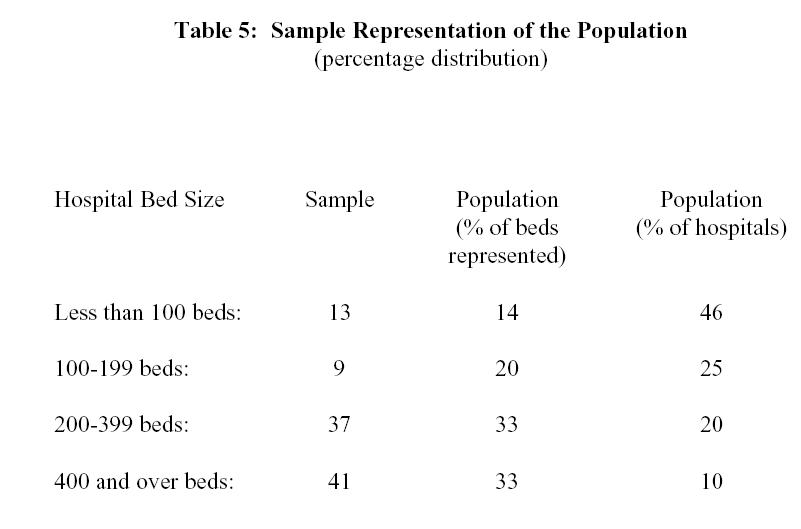
It must be recognized that the sample of hospitals included in the study may not be a representative sample of all US hospitals. Many of the smaller hospitals returned the survey indicating that the survey was not relevant to them. Oftentimes, smaller hospitals, particularly the ones located in rural areas, may not be organized to facilitate the marketing function and, as such, may feel that the study is not relevant to them. These limitations on generalizability should be recognized. Yet, the interrelationships between variables relevant to relationship marketing shed some light on relationship marketing practices and their impact on performance indicators. The results may still be relevant to smaller hospitals as they are increasingly being acquired by large hospitals and corporate organizations who in turn would direct or influence a more sophisticated marketing approach in these small hospitals. It may further be noted that hospitals with less than 100 beds represent nearly 43 percent of the total US hospital population but account for only 12.5 percent of the beds. Larger hospitals (300 beds or more) represent 18 percent of hospitals and account for nearly 50 percent of beds. Representativeness of a sample may be based on number of hospitals or number of beds and may primarily depend on the study’s purpose. In Table 5, a comparison of the study sample with the population of US hospitals is shown.
Another limitation of the study is that the data on hospital performance represents year 1993, whereas the survey was conducted in August 1994. Although many hospitals would have instituted various partnering programs at different times over the last three-to-four years period, there may be a time lag between such programs were activated and when it impacts performance. Assuming that the impact of relationship marketing programs is expected to be generally in the long-term than short-term, the success or failure of certain programs may not be fully captured in this study. Another limitation is that the success measures used here are based on the application of relationship marketing in the old paradigm of occupancy rates, gross revenues, admissions per bed, etc. Many will argue that in the new paradigm, success should be measured in terms of improving the health status of a particular community of people, access and delivery goals accomplished, patient satisfaction achieved, clinical outcomes, etc. Recognizing this limitation, one is cautioned against drawing generalized conclusions on relationship marketing and hospital success based on the results of this study. However, assuming the absence of any other major initiatives, relationship marketing activities and partnering programs are indirectly identified as influencing the performance indicators of a hospital.
Implications and Suggestions for Future Research
Future research can build on and expand the ideas presented here. The first obvious move could be to conclusively test the propositions implied by this study. One can also study the underlying reasons as to why some specific programs produce better results than others and if there is any effect of the relationship management characteristics that significantly impacts results. For example, relationship marketing programs may be more successful when there is open communication, mutual commitment, operational alignment, mutual understanding of each otherís goals, etc. between the partners. Are these characteristics common across successful partnering with customers, suppliers, payers, and providers. Why does partnering with suppliers not yield significant results for hospitals?
Research to study the impact of interrelationship between managed care and relationship marketing would be very useful. For example, how can relationship marketing improve the financial performance of a health plan or integrated delivery system under capitated reimbursement? Does relationship marketing aimed at insurance points have an influence on patientís decision to stay with current health plans or switch plans.
Finally, research that takes the user or consumer perspective of measuring the success or failure of relationship marketing programs will be most welcome. The effectiveness depends upon how consumers/users respond to these relationship marketing programs of the hospital. To what extent consumers are aware, consider the program features as importance, and the extent to which they use it and related services, indicates the success or failure of programs. Specially, in the new paradigm when experts and industry observers increasingly professing that the success of health care must be assessed on the basis of the community is health status, patient satisfaction, etc., the consumer approach to measuring performance becomes very relevant. In the future, reliable instruments and standardized measurements of hospital performance on these variables will be most welcome.
Managerial Implications
As competition intensifies in the hospital market, drop in customer loyalty is likely to become steeper unless hospitals place emphasis on patient satisfaction (Jones and Sasser, 1995). One way hospital systems are going to respond to the growing competition is by engaging in relationship marketing activities and by partnering with their suppliers and other health care providers, including competitors. Thus, the answer to intense competition is not rivalry but cooperation. By developing cooperative relationships with customers, suppliers and other health care providers, hospital systems can overcome the challenges of competitive threat. Similarly, it can also be implied that in order to rapidly engage in relationship marketing activities hospital systems must become more market and marketing-oriented because such orientation is likely to foster the adoption of relationship marketing and partnering programs.
Many hospitals in the US are engaged in the practice of relationship marketing. The larger the hospital, the more the likelihood that it is implementing a higher level of relationship marketing programs. Although the objectives for developing partnerships with customers, suppliers and other health care providers differ, the primary focus is to meet or exceed customer expectations in service quality, and delivery. While results of these efforts are likely to be long term, the study indicates that those hospital systems that are engaged in relationship marketing have superior performance in such areas as, occupancy rates and better cash flows. Relationship marketing programs with customers seem to be the most effective followed by partnering programs with providers. The impact of relationship marketing programs with suppliers tends to be anemic with respect to hospital performance indicators used in this study. As hospitals struggle to survive in the changing landscape for health care, initiation and successful management of relationship programs with customers and providers may enhance their likelihood for survival and success.
Results presented in Table 3, can be used by managers and other decision-makers to improve their hospitalís performance. For example, to enhance occupancy rate, hospital systems can engage in the use of database marketing, cross-selling of services to regular customers, design network and membership benefit programs for customers, engage in joint marketing with other health care providers, or establish joint ventures and alliances with them. Similarly, for increasing admissions per bed which is an important indicator of success in a highly managed care market, such relationship marketing programs as after-marketing services, ongoing relationship with HMOs, PPOs, physician groups and payers, as well as programs identified for the enhancement of occupancy rates are recommended.
In order to increase net income margin, relationship with patients and the use of database marketing are likely to yield the best results. However, any gains in improving net income margin through these efforts may be frustrated by the existence of managed care relationships with HMOs/PPOs/IPAs and payers who receive deep discounts. Gross patient revenue per patient day could be significantly increased through ongoing relationships with all groups of customers, by the use of database marketing and cross-selling activities and through cooperative management of logistics with other organizations. To improve total profit margin, hospitals are best advised to develop and maintain on-going relationship with patients and use database marketing programs. Finally, to reduce the uncollectible ratio, post treatment satisfaction and after-marketing activities could be started along with the formation of joint ventures and alliances with other health care providers.
References
American Hospital Association, AHA Guide. 1994.
American Hospital Association, Hospital Statistics: The AHA Profile of United States Hospitals. 1994-95.
Berry, Leonard L., Relationship Marketing of Services — Growing Interest, Emerging Perspectives, Journal of the Academy of Marketing Science 23 (Fall 1995): 236-245.
Boyle, Brett F., Dwyer, Robert, Robicheaux, Robert A., and Simpson, James T., Influence Strategies in Marketing Channels: Measures and Use in Different Relationship Structures,
Journal of Marketing Research 29 (November 1992): 462-73.
Cassidy, Judy, et. al., Critical Relationships in Integrated Delivery, Health Progress, (December, 1993): 38-55.
Crosby, Lawrence A. and Stephens, Nancy, Effects of Relationship Marketing on Satisfaction, Retention, and Prices in the Life Insurance Industry, Journal of Marketing Research 24 (November 1987): 404-411.
Crosby, Lawrence A., Evans, Kenneth R., and Cowles, Deborah, Relationship Quality in Services Selling: An Interpersonal Influence Perspective, Journal of Marketing 52 (April 1990): 21-34.
Doyle, Stephen X. and Bondreau, James G., Hospital-Supplier Partnership, Journal of Health Care Marketing, 9 (1) 1989: 42-47.
Dunn, Dan T. Jr., and Thomas, Claude A., Partnering with Customers, Journal of Business and Industrial Marketing, 9 (1) 1994: 34-40.
Dwyer, F. Robert; Schurr, Paul H.; and Oh, Sejo, Developing Buyer-Seller Relationships,
Journal of Marketing, 51 (April 1987): 11-27.
Eccles, Robert G., The Performance Measurement Manifesto,” Harvard Business Review, 69 (January-February 1991): 131-137.
Ganesan, Shankar, Determinants of Long-Term Orientation in Buyer-Seller Relationships, Journal of Marketing, 59 (April 1994): 1-19.
Gould, Stephen J., Macrodynamic Trends in Health Care: A Distribution and Retailing Perspective,” Health Care Management Review, 13 (2) 1998: 15-22.
HCIA, Inc., and DeLoitte and Touche LLP, The Comparative Performance of US Hospitals: The Source Book, DeLoitte & Touche LLP., Chicago, Il. 1995.
Johanson, Jan; Lars Hallen; and Seyed-Mohammed, Nazeem, Interfirm Adaptation in Business Relationships, Journal of Marketing, 55 (April 1991): 29-37.
Jones, Thomas O., and Sasser, W. Earl, Jr., Why Satisfied Customers Defect, Harvard Business Review, 73 (November-December 1995): 88-99.
Kalwani, Manohar, and Narayandas, Narakeswari, Long-Term Manufacturer-Supplier Relationships: Do They Pay Off for Supplier Firms? Journal of Marketing, 59 (January 1995): 1-16.
MacStravic, R. S. Marketing by Managing Relationships, Health Progress,. 65 (9) 1984: 49-51, 60.
MacStravic, R. S., and Denning, E., Relationship Marketing in Maternity Care, Journal of Hospital Marketing, 7 (Fall/Winter 1986): 115-123.
McDermott, Dennis R.; Franzak, Frank J.; and Little, Michael W., Does Marketing Relate to Hospital Profitability? Journal of Health Care Marketing, 13 (2) 1993: 18-25.
Morgan, Robert M., and Hunt, Shelby D., The Commitment-Trust Theory of Relationship Marketing, Journal of Marketing, 28 (July 1994): 20-38.
Naidu, G. M., Relationship Marketing in Health Care Industry, in Relationship Marketing: Theory, Methods and Applications, Jagdish N. Sheth and Atul Parvatiyar, eds., Center for Relationship Marketing, Emory University, Atlanta, GA. 1994.
Naidu, G.M.; Narayana, Chem L.; and Pillari, George D., Marketing Parallax in Health Care Industry: An Empirical Study of Hospitals, Journal of Hospital Marketing, 6 (1) 1991: 5-27.
Naidu, G.M.; Kliemenhagen; Arno; and Pillari; George D., Is Product-Line Management Appropriate for your Health-Care Facility, Working Paper, College of Business, University of Wisconsin-Whitewater. 1994.
O’Connor, Stephen J.; Shewchuk, Richard M.; and Carney, Lynn W., The Great Gap: Physicians’ Perceptions of Patient Service Quality Expectations Fall Short of Reality, Journal of Health Care Marketing, 14 (2) 1994: 32-39.
Parvatiyar, Atul, and Sheth, Jagdish N, Contemporary Knowledge of Relationship Marketing, Center for Relationship Marketing, Goizueta Business School, Emory University, Atlanta, GA. 1996.
Paul, Terry, Relationship Marketing for Health Care Providers, Journal of Health Care Marketing, 8 (3) 1988: 20-25.
Peppers, Don, and Rogers, Martha, The One to One Future, Doubleday, New York, NY. 1993.
Reichheld, Frederick F., and Sasser, W. Earl, Zero Defections: Quality Comes To Services,
Harvard Business Review, 68 (September-October 1990): 105-111.
Sheth, Jagdish N., The Domain of Relationship Marketing, paper presented at the Fourteenth AMA Faculty Consortium on Relationship Marketing, June 9-11, 1994, Atlanta, GA.
Sheth, Jagdish N., and Parvatiyar, Atul, Towards a Theory of Business Alliance Formation,
Scandinavian International Business Review, 1 (3) 1992: 71-87.
Sheth, Jagdish N., and Parvatiyar, Atul, Relationship Marketing in Consumer Markets: Antecedents and Consequences, Journal of the Academy of Marketing Science, 23 (Fall 1995): 255-271.
Sheth, Jagdish N., and Parvatiyar, Atul, The Evolution of Relationship Marketing,
International Business Review,. 4 (December 1995): 397-418.
Sheth, Jagdish N., and Sisodia, Rajendra, Improving the Marketing Productivity, in Marketing Encyclopedia: Issues and Trends Shaping the Future, Jeffrey Heilburnn, ed., American Marketing Association, Chicago, IL. — NTC Business Books, Lincolnwood, Il. 1995, pp. 217-237.
Trombetta, William L., Channel Systems: An Idea Whose Time Has Come in Health Care Marketing, Journal of Health Care Marketing, 9 (September 1989): 26-35.
Turner, Paul D., and Pol, Louis G., Beyond Patient Satisfaction: Broaden the Scope of Quality Measurement by Integrating the Marketing View with Other Perspectives, Journal of Health Care Marketing, 15 (3) 1995: 45-53.
Vavra, Terry G., Aftermarketing: How to Keep Customers for Life Through Relationship Marketing, Business One Irwin, Homewood, Il. 1992.
Wagner, Henry C.; Fleming, David W.; Mangold, Glynn; and Laforge, Raymond W., Relationship Marketing in Health Care, Journal of Health Care Marketing, 14 (4) 1994: 42-47.
Weitz, Barton A., and Jap, Sandy D., Relationship Marketing and Distribution Channels,
Journal of the Academy of Marketing Science, 23 (Fall 1995): 305-320.
Wilson, David T., An Integrated Model of Buyer-Seller Relationships, Journal of the Academy of Marketing Science, 23 (Fall 1995): 335-345.